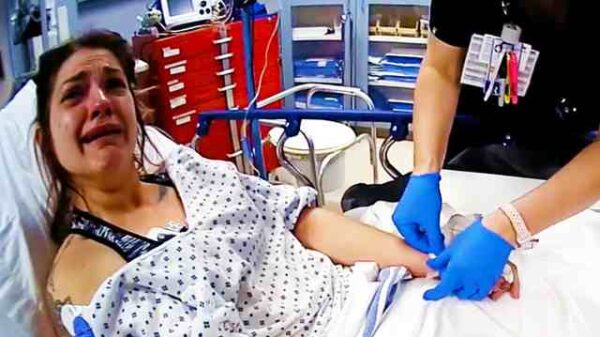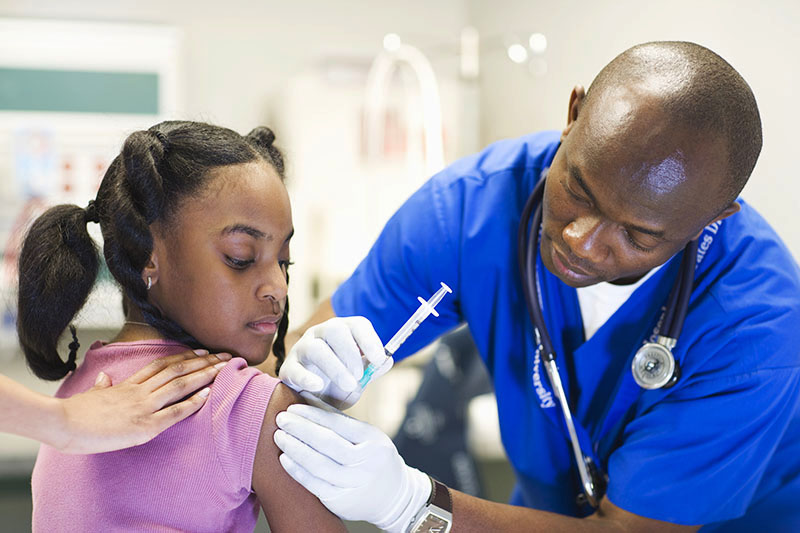
ER Productions Limited/Getty Images
The American Medical Association’s new accreditation guidelines suggest genetic testing of Black patients is racist – and such testing must end.
The AMA and the Association of American Medical Colleges (AAMC) are the same groups that recently released a new “Health Equity” guidance banning common terms such as “morbid obesity.”
READ ALSO: American Medical Association Cancels ‘Morbid Obesity,’ ‘Inmates,’ ‘Homeless’
The AMA and AAMC claim genetic testing of minority patients is racist and can “create harm” and “leads directly to racial health inequities.”
However, some medical conditions disproportionately affect minorities, such as Blacks, Hispanics and Jews.
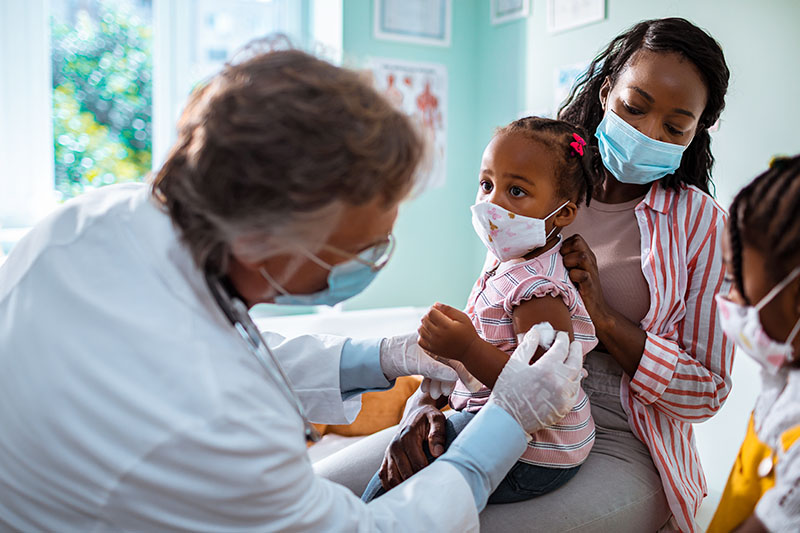
Marko Geber / DigitalVision
Sickle cell anemia is more common in people of African descent (8 of 10 sickle cell patients are Black). The sickle cell trait can also affect Hispanics.
The AMA and AAMC also recommended that the licensing exam for new doctors change from numerical scoring to pass-fail.
A group of Black doctors and professors warn that the new accreditation guidelines puts minorities and the general public at risk of serious harm or death.
Five black professors told the New England Journal of Medicine in March, that denying genetic race testing is “a form of naive ‘color blindness’” that would “perpetuate and potentially exacerbate disparities.”
Jeff Singer, a general surgeon in Arizona, says “A lot of conditions,” such as triple-negative breast cancer, which disproportionately affects Black women – “vary based on genetics. We’re talking about matters of life and death here.”
Singer argues that the AMA and AAMC’s accreditation guidance will result in doctors who are under qualified and put lives at risk.
“They’re trying to superimpose social science onto medical science,” Singer said. “But as a consumer of health care, I’d just like to know that whoever is treating me is qualified. Because my life is on the line.”
![]()